Reducing patient non-compliance

I am a registered nurse at the Department of Urology’s Outpatient Section of the Counties Manukau Health (CM Health) in Auckland, New Zealand, and I would like to share my insights regarding the value of teamwork and a nurse-led appointment management system for prostate biopsies.
CM Health is one of three District Health Boards in Auckland, serving an estimated population of 512, 000 people, or about 11% of New Zealand’s total population. CM Health’s population includes high numbers from New Zealand’s indigenous people, namely Maori (16%) as well as Pacific (23%) and Asians (22%). These unique ethnic groups challenge us as health care professionals to continuously examine our procedures and practices to ensure that we provide optimal care across all cultural groups. In this article, I would attempt to describe a quality project I have been involved with at CM Health.
Male patients referred by their general practitioners to CM Health urology service with elevated PSA and/ or irregular prostate on digital rectal examination are seen at outpatients clinic by a urologist for an informed consent discussion regarding whether they wish to consider a transrectal ultrasound (TRUS) guided prostate biopsy. If a decision is made to proceed to prostate biopsy, the patient’s records are placed on the biopsy waiting list and he returns at a later date for the procedure. Before he leaves the urology consultation he will be given a patient information sheet regarding the planned biopsy procedure and a rectal swab will be taken and sent to the laboratory to be tested for the presence of extended-spectrum bèta-lactamase (ESBL) and ciprofloxacin resistant bacteria.
At CM Health TRUS biopsies are performed once a week by a radiologist. Patients are required to undergo a basic coagulation screen and midstream urine sample seven days prior to the procedure. Patients on anticoagulant medication are given instructions as to when to stop their medication prior to the biopsy, and oral antibiotics are prescribed in accordance with their rectal swab results (if no resistances are detected the standard prophylaxis is one gram of oral ciprofloxacin one hour prior to the appointment). Men scheduled for a prostate biopsy are required to be accompanied to their appointment who can drive them back home following the procedure. If any of these requirements are not followed the patient risks a delay or a re-scheduling of the appointment.
At the beginning of 2012 CM Health urology nurses recognised that there were a significant number of TRUS biopsy clinic slots that were not being utilised. Closer investigation revealed that in fact only 80% of the available clinic slots were being used, with wasted appointments mainly due to poor patient compliance or preparation for the prostate biopsy appointment. When analysed by ethnicity, Pacific Island men were at the highest risk of cancelling their own biopsy appointment or having their biopsy cancelled by a health care professional.
In September 2012, in response to our heightened awareness of the cancellation risks Pacific men faced, the urology team met with the CM Health’s Pacific Health Unit (PHU) to explore the nature of barriers that may be contributing to Pacific Island male patients missing their biopsy appointments. This process identified multiple issues including language difficulties, a tendency to avoid health care appointments until symptoms worsened, a lack of understanding regarding procedures and potential diagnoses, and fear and anxiety related to the biopsy procedure.
The CM Health team then explored possible solutions, using available resources, to the issues identified. This process included contacting colleagues in other urology departments to discuss our issues and seek information regarding their prostate biopsy protocols. We also completed a literature review on the relevant topics.
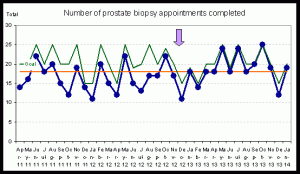
Figure 1: Goal (green line) and actual number of prostate biopsy appointments completed (blue line) with the arrow indicating the moment of starting with the new strategy
Identifying potential barriers
As a result of these processes, we reviewed our appointment letter and patient information sheet for TRUS Prostate Biopsy and updated the content to provide clearer information. We put in place a process where the PHU would contact all Pacific male patients with a planned appointment for a prostate biopsy to enable us to offer support, reinforce instructions and communicate with the patients in their native language when needed. The PHU staff would then liaise as required with the urology clinic nurses to iron out any potential barriers identified for Pacific Island male patients.
In November 2012, a urologist and a radiologist met with urology nurses to discuss best practice guidelines regarding TRUS prostate biopsy. In particular our guidelines were reviewed within the context of “when not to proceed with a scheduled prostate biopsy” so as to minimise both patient risk and last-minute cancellations. A systematic nurse-led process was also established for reviewing rectal swab results, ensuring that a prescription for the correct antibiotic is delivered in a timely manner to every patient.
Review of outcomes following implementation of these collaborative strategies indicates greater engagement with our Pacific Island patients as well as a significant improvement in the overall use of TRUS prostate biopsy appointments. Data from 2013 indicates that 95% of scheduled prostate biopsy appointments proceeded on the day. The challenge now is to sustain this improvement over the long-term and to continue to look for ways of improving our patient-centred outcomes. As the maxim goes: “Alone we can do so little; together we can do so much”
Tanja Rogers, RN
Counties Manukau Health Urology Dept.
Auckland (NZ)
Tanja.Rogers@cmdhb.org.nz